This post is also available in:
Hello Warriors!
Following two huge victories in my particular battle in The Netherlands at the University Medical Center of Groningen and in the second epic edition of the “Battle of los Alamos” I cannot stop celebrating our achievments both with Dr. Derks and his team in the Hospital and with all my Warriors In Action in our last Charity Hiking in which we raised more than 6000 USD to support GSD research.
Among all these emotions, I realized that I never had the time to tell you how demanding my daily battles were before I got the new treatment. I think it is now a good moment to do it and when I tell you about what we did in Groningen and my new routine you will better realize the huge difference.
So, without futher ado, this is how a standard day was:
09.00 am: Wake up. Prepare 3 baby bottles of 210 ml of soy formula milk (210 ml of water and 7 spoons of powder soy formula milk) for the day. Check blood sugar. Stop continuous night feed and get Nina off the feeding pump. Check blood sugar. Give 60 ml soy formula milk. If she does want to eat by mouth give it to her by nose-gastric tube. Clean the feeding pump with water
09.25: give 50 mg of Allopurinol dissolved in a spoon of water by mouth.
09.45 am: check blood sugar and give 60 ml soy formula milk. Give a bath which cannot last more than 40 minutes. Before bathing, cover with a plastic bag the continues glucose monitoring device in her upper
arm. This device helps us to understand trends: whether the blood sugars are going up or down, but we cannot trust it very much regarding accurate BS figures. For that, it is better to use the glucose meter and get the result directly from blood.
10.20 am: check blood sugar and give 60 ml soy formula milk or 5gr of sugar-free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
10. 35 am: Give her 20 grams of raw cornstarch. If she does want to eat by mouth give it to her by nose-gastric tube and wash the tube down with 5 ml of water after. The cornstarch, being a slow-absorption carbohydrate, is supposed to help keeping BS stable for a longer time. However, in Nina’s case, it was not working properly, apparently because of a serious absoption problem.
10.50 am: try to give soya yogurt or a piece of small sausage to bite or any other piece of food she might want to try (90% of the cases: she does not eat anything by mouth). It is extremely important to continue trying till one day she manages. Whenever she is able to eat by mouth we will be in a position to remove the NG tube and it will be much better to get real food than formula milk or other fluids.
11.05 am: check blood sugar and give 60 ml of soy formula milk. If she does want to eat by mouth give it to her by nose-gastric tube. Try to make her eat something by mouth.
11.15 am: give 6 ml of vitamin E (by mouth); The vitamin E supplementation, as an antioxidant, reduce the number of neutrophils deaths so that the neutrophils count is increased and their function is improved.
11.20 am: Ups, scary moment of the day. The neupogen (filgastrim) daily shot. We take the neupogen vial from the fridge and load a syringe with 21 micrograms. It is normally injected in the upper leg, on a daily basis. Neupogen helps to increase the neutrophil count as well.
11.50 am: give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
12.35 pm: 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
12.40 pm: prepare baby food – weight every single ingredient to obtain a semi-liquid puree (total of 10 grams carbohydrates and 40-50 grams of proteins + 5 gr of extra-virgin olive oil each portion)
01.15 pm: check blood sugar. Try to give the baby food. At 50% of the times she will not eat it or it might take 30 minutes for 3-5 spoons. In case after the first 10 minutes of try she does not eat it at all, give 60 ml of soy formula milk.
01.55 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
02: 10 pm: Give her 20 grams of row cornstarch. If she does want to eat by mouth give it to her by nose-gastric tube and wash the tube down with 5-10 ml of water after.
02: 15 pm: It is time for a nice Mediterrean SIESTA!!!
02. 40 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth or if she is sleeping, give it to her by nose-gastric tube.
03. 25 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
04:10 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
04:25 pm: Give her 20 grams of row cornstarch. If she does want to eat by mouth give it to her by nose-gastric tube and wash the tube down with 5 ml of water after.
05:10 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube. Try to give her anything she can eat (protein or small pieces of carbohydrates like rice crackers, corn soft crackers, soya yogurt, or anything else she can try to chew)
05:55 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
06: 40 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube. Try to give her anything she can eat (protein or small pieces of carbohydrates like rice crackers, corn soft crackers, soya yogurt, or anything else she can try to chew)
07.20 pm: check blood sugar. Try to give the baby food (previously prepared and kept refrigerated, otherwise prepare one measuring all ingredient, cooking and smashing as liquid puree). At 50% of the times she will not eat it or it might take 30 minutes for 3-5 spoons. In case after the first 10 minutes of try she does not eat it at all, give 60 ml of soy formula milk.
An alternative if she does not eat any real food during the day is to try to give it through siringe by NGtube and wash the nouse-gastric tube down with 15 ml of water after that. If it gets clogged (and she does not drink the formula by mouth) we are in trouble and we have to take some of the tube out off her nose and try to flash it with warm water. If it does not work we need to remove the tube and quickly replace it with a new NGtube (taping it in her face with two special types that need to be cut) before the fasting time is over and she goes into hypoglycemia.
08.05 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
08: 20 pm: Give her 20 grams of row cornstarch. If she does want to eat by mouth give it to her by nose-gastric tube and wash the tube down with 5 ml of water after.
08.50 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
09.35 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
10.20 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
11.05 pm: check blood sugar. Give 60 ml of soy formula milk or sugar free cereals in 80 ml of water. If she does want to eat by mouth give it to her by nose-gastric tube.
11.15 pm: prepare three baby bottles (about 700 ml) of soya milk and cereals (all measured with a scale as usual) for her night continues feed. Put inside her bottles 5 drops of vitamin D, 1 ml of Iron, 10 drops of sugar-free multivitamin, a capsule of Omega 3 (open it through a middle and squeeze the liquid into the bottle), and one probiotic.
11.50 pm: check blood sugar. Give 60 ml of soy formula milk and connect Nina to the pump to feed her continuously at 50 ml/h rate. Check Nina blood sugar closely the first hour and then continue every hour approximately. If her bs drops less than 60-70 blood glucose, or go higher than 110 bs, increase or decrease the speed of the pump.
If the cereals got stuck in the system, the pump alarm ring and we need to wake-up and solve the problem. If Nina moves during the night the pump can get clogged and again the pump rings, so we need to sort out the issue. If Nina experience a drop in her blood sugar during the night she wakes up, in most of the cases she is hypoglycemia unaware and that is why is very important to keep monitor her day and night.
This is until 09.00 am when the routine starts, all need to be repeated the above all over again.
On top of all that, keep into consideration:
Every time we use a syringe for feeding Nina through tube, it needs to be wash.
Every now and then, during the day, do syringe-maintenance (wash them and put olive oil to avoid the plastic to expand and get stuck – syringes cannot be bought in quantity, they are provided counted in number).
Get ready in advance soya formula or cereal baby bottles during the day when needed – just prepare the dried empty baby bottles with the measured powder (dry well the baby bottles with a piece of paper to avoid humidity that can cause the powder to get stuck) and remember to take about 15 minutes to prepare the night feeds as well if time allows.
Nina needs to be changed very often due to the large amount of liquid she drinks all day long but also keep into consideration that raw cornstarch causes blend stools/diarrhea several times during the day. Nina plays all day long, so all treatments needs to be given during her daily routine. If Nina walks more than 10 minutes in a row we need to stop and sit her for a while (she cannot run i.e. cause she is burning too much sugar due to lots of energy consumption) or her glucose level will drop very fast and she might last less than 40-45 min, like 20 min.
Emergencies
If Nina get sick, she has a bacterial or virus infection, her glucose levels drop, or her fasting time is less than the 40-45 min above described so we need to monitor closely if the situation deteriorates and she might need to go to the hospital to give glucose intravenous to keep her glucose level stable. If the infection involve her gut, or if she has vomit or diarrhea, this is an emergency cause her glucose level does not arise and she needs to be taken to the hospital to get glucose intravenous otherwise she can have seizure in few minutes that can cause brain damage or even die (and always cause consequences or damages to the organs due to the raise of lactic acid, tryglicides, transaminase, etc).
If Nina get a cold, due to the BGtube she can vomit even 10 times a day. Every vomit can cause a severe hypoglycemia in few minutes so need to be monitored closely to understand if the cause needs to be addressed immediately at home or if there is need to go to the hospital: give her medicines to stop it if she vomits more than twice, give glucose if her glucose level drops, bring her to the hospital is she does not stop or cannot keep her glucose level stable at home.
Whenever Nina goes to the hospital it is a huge challenge for nurses to find a vein to canalize. She has thin veins and also, she has been canalized many times as much as she undertakes periodic blood exams so that her veins are broken / enable to serve this purpose due to phlebitis, etc. Very often she ends up in intensive care (under anesthesia) and a central vein to be taken. One more reason why deciding to take a central vein is because of safety and life-saving reasons (for instance, if she suffers from an infections whereby her life depends on glucose intravenous because she cannot eat, her intestine would not absorb any food to keep her glucose stable), she needs to get a more secure intravenous access to avoid any life-threatening risk.
Diet
Nina cannot (and will never eat in her life) eat any type of sugar: fructose, lactose, galactose. She cannot eat fried food nor processed food or alcohol. When she eats carbohydrates they need to be measures in grams, given in a due time and eaten in a due time. Nina is free to eat only proteins any time and without any limitations except for what above said.
Emergency bag
Nina can touch and through away her ngtube during the way or by night: we need to monitor if this is the case and have always an emergency ngtube on the emergency bag + two different types of stripes for the face. Nina’s glucose monitor can fail: she needs to carry a sensor replacement + stripes + 2 types of bandages to cover her arm.
Nina needs to be checked glucose levels all the time, she needs glucose stripes, glucose hand device, niddles, cotton pads and hand-sanitizer.
Emergency bag includes extra stripes, extra syringes of all types (for soya milk, for medicines, for daily injection), glucose gel, dextrose 10% in a small glass bottle, a few small containers of soya milk and cereals (to last at least 6 hours), water, gauzes, nouse-gastric tube. Always bring Nina’s emergency protocol letter into her bag.
So, I have already told you a lot of things and I still have the feeling that I forgot something 🙂
In any case, this is my “boring diary” but it is also the one that kept me alive.
My “funny diary” is everything else: musical books, painting, playing, clay, play dough, dancing, singin, walking around… and a lot a lot of love from all of you plus all the initiatives that the Warriors In Action are implementing!





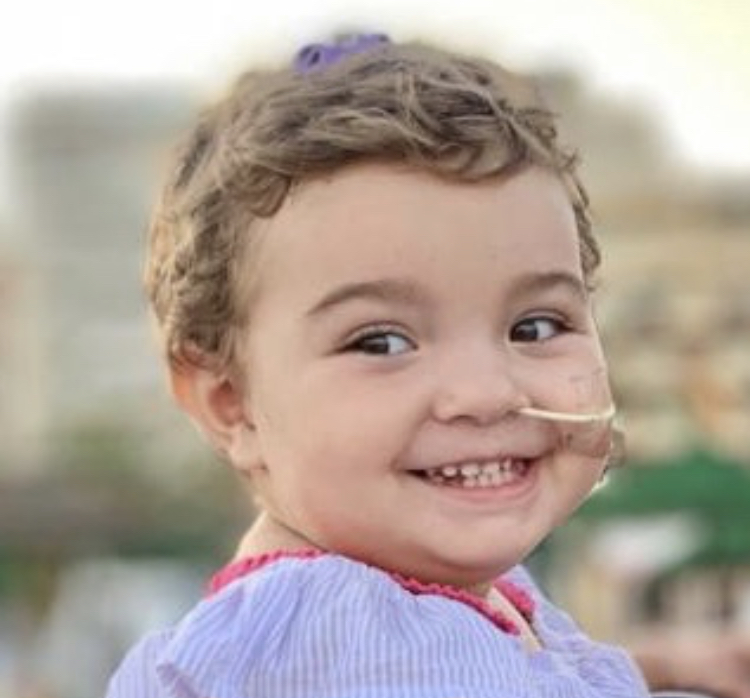





❤️ diary of a warrior ❤️ hourly battles, wonderful allies and some magic powers: your wonderful smile and your incredible parents ❤️